Rory's Story
Rory Miller, 50, is a full-time district fire chief with the St. Bernard Fire Department and is also a paramedic. He and his wife, Jessica, are the proud parents of two daughters and live on a 20-acre farm.
On New Year’s Eve, Rory began to feel ill at work. He went to a local clinic for a COVID-19 test, which came back positive. Five days later, he started to feel worse and experienced a coughing fit that triggered his reactive airway disease. Unable to get his cough under control, Rory’s wife rushed him to Ochsner Medical Center - Northshore.
Rory was admitted to the hospital and placed on a BiPAP machine, a non-invasive device that helps push air into the lungs. He responded well and discharged home. A few days later, he began experiencing pain and tingling in his lower legs and was unable to lift his arms. Concerned, he returned to the hospital, where he was readmitted and diagnosed with Guillain-Barre syndrome, a disease that attacks the nerves of the body’s extremities. In Rory’s case, it ascended from his feet to just below his diaphragm. Because of this, he had difficulty standing, walking and maintaining an upright posture. After experiencing a seizure, Rory was transferred to Ochsner Main Campus in New Orleans for further evaluation and treatment. He remained there for several weeks before stabilizing for a transfer to Northshore Rehabilitation Hospital.
When Rory arrived, he couldn’t walk and was experiencing foot drop (difficulty lifting the front part of the foot) and had no sensation in either leg. His physical and occupational therapists worked together to find a balance between doing enough to facilitate progress, but not too much out of concern of overloading his muscles which can cause a reverse reaction, decreasing muscle strength. He was also still experiencing generalized weakness from the COVID-19.
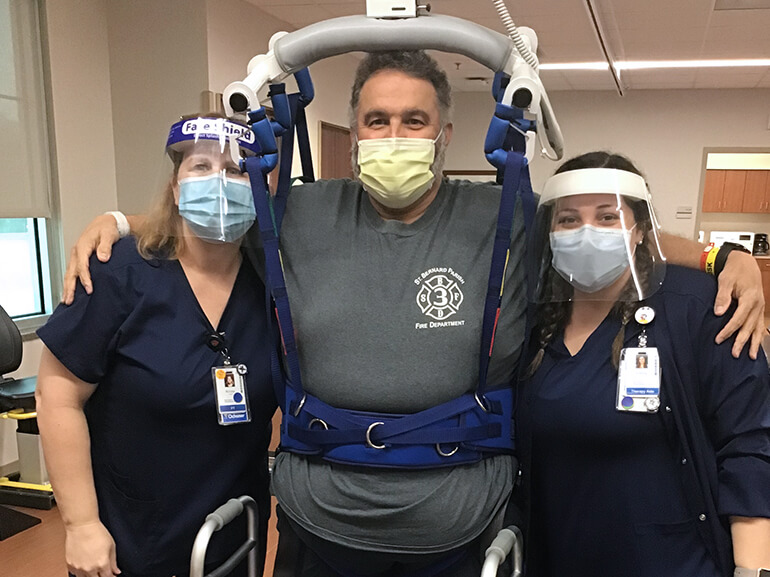
To start his physical therapy journey, Rory was placed in an overhead harness system that provided support while he worked on walking four to five feet. He also focused on standing balance activities and various leg exercises with resistive balls and therapy resistance bands. Once his legs were strong enough, Rory progressed to using a rolling walker and practiced walking often, eventually reaching over 150 feet with minimal assistance. He was also issued ankle foot orthotics, specialized braces that provide support and stability, to assist with his ability to lift his toes up during walking.
During his occupational therapy sessions, Rory was taught how to safely get dressed by focusing on locking his knees during standing. He also participated in upper body strengthening using resistance bands, free weights and the arm bicycle. All of this provided Rory with the ability to regain some of his independence.
Rory’s illness and rehabilitation experience had a considerable impact on both his physical and mental well-being. He recalls a turning point when his body began responding more to treatment, “I started to make significant leaps and bounds in therapy.” He also regained muscle movement and control in his legs and feet, but it was an emotional fight. “The psychological battle was much harder than the physical battle,” said Rory. “I enjoyed going to therapy because I got out of my head and could focus on recovery.”
After 18 days at Northshore Rehabilitation, Rory made significant progress walking more than 150 feet and maneuvering hallway turns and taking backward steps to get into the car.
Upon discharge he shared, “I’m looking forward to seeing my family – to hug my kids and my wife and to be home with them.”